Macular Degeneration
Nobody walks into an eye appointment expecting bad news. You figure your vision is fine, maybe a little blurry here and there but nothing serious. Then the doctor pulls up a scan and points to a spot right in the middle of your retina. Something is breaking down in there. And suddenly you are hearing words like age-related macular degeneration for the first time, trying to make sense of what that even means while you are still sitting in the chair.
Here is what I wish more people knew before that moment. Macular degeneration does not show up overnight. It has probably been doing its thing for months, maybe years, before anyone catches it. Most people walk around with early macular degeneration and have absolutely no clue. No pain. No obvious signs. Nothing feels off until one day it does.
Macular degeneration is a common eye disease that affects a part of your eye called the macula. The macula sits right in the center of your retina, and it handles all your detailed vision. Reading. Driving. Seeing someone’s face across a table. That is your macula doing the work. When macular degeneration starts wearing it down, that central vision goes fuzzy, or wavy, or just… gone in patches. Meanwhile the edges of your vision, your peripheral sight, usually stays okay. Which almost makes it worse because you can tell something is wrong but you can still sort of see.
The full name is age-related macular degeneration, or AMD for short. It is the leading cause of serious vision loss in older adults. AMD affects people over 50 the most, and your risk keeps climbing every year after that. If you have hit 60 or 70, this is not some rare thing. It is common. Really common.
At Honor Wellness in Vancouver we treat macular degeneration patients who are fed up with the “wait and see” approach. We use ophthalmic acupuncture alongside your existing care. It does not replace your injections or whatever else your doctor has you on. It fills in the gaps those treatments leave open.
What Is Age-Related Macular Degeneration?
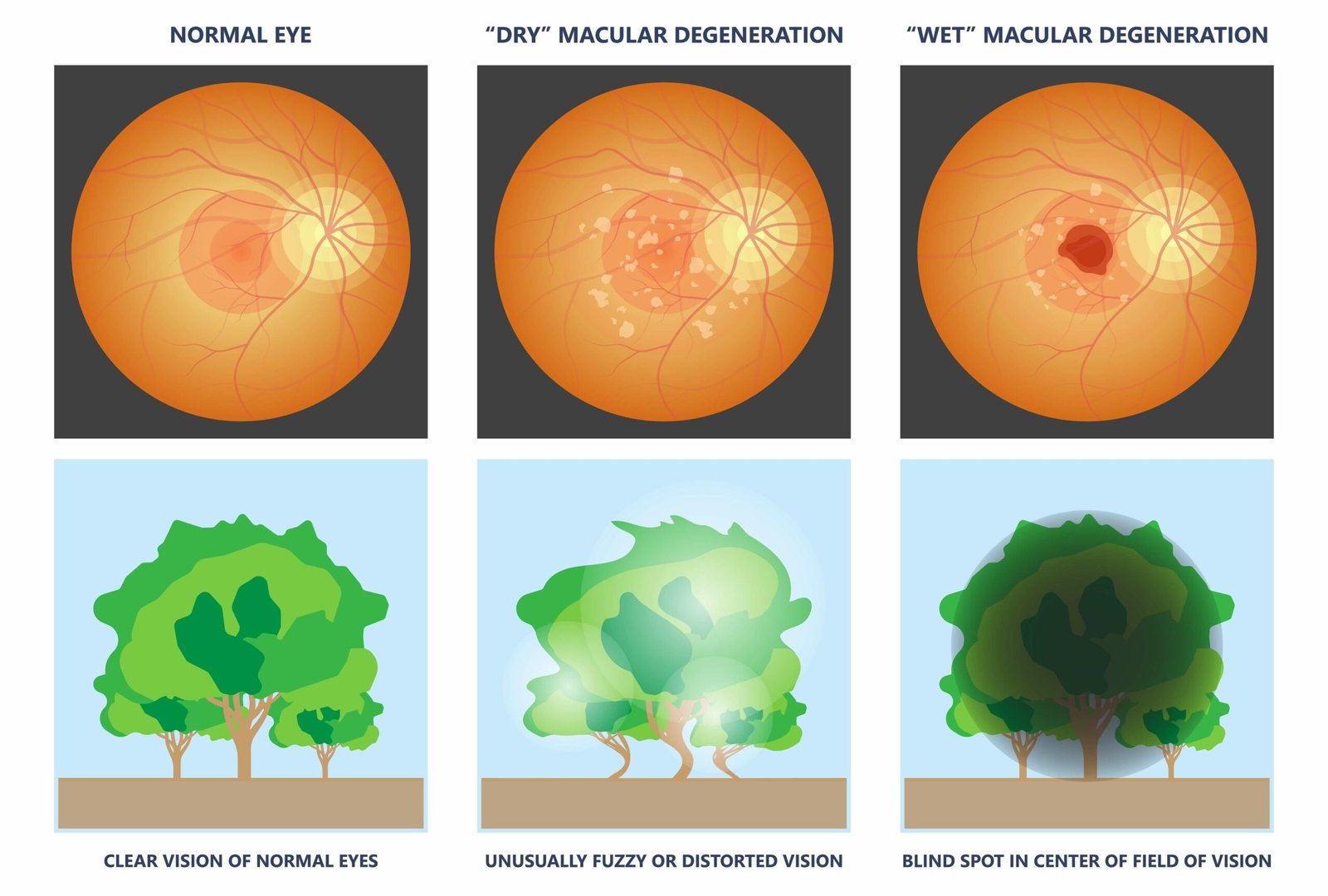
Okay so picture this. Your retina is like a screen at the back of your eye. Light hits it and your brain reads that light as an image. The macula is a small spot right in the middle of that screen, and it is responsible for all the sharp, focused stuff you see. When macular degeneration shows up, that spot starts falling apart. Cells die off. Things get blurry right in the center of whatever you are looking at.
Age-related macular degeneration is an eye disease that affects central vision. It is also an eye condition that causes blurred vision, and it is an eye disease that may get worse over the years. For some people it creeps along slowly. For others it picks up speed. A lot depends on which type of macular degeneration you are dealing with.
There are two types and they behave very differently.
Dry macular degeneration. This is the one most people get. Also called dry ARMD. About 80 to 90 percent of age-related macular degeneration cases fall into this category. What happens is the macula thins out as you age. Little protein deposits called drusen pile up underneath the retina. Slowly, over years sometimes, this causes atrophy. The macular cells just waste away. Dry AMD moves at its own pace. Some folks barely notice changes in their vision. Others lose quite a bit. Right now there are no drugs that reverse the damage from the dry form, but certain supplements like the AREDS2 formula can slow things down for some people.
Wet macular degeneration. Less common, way more aggressive. Your doctor might call it neovascular ARMD or wet AMD. What makes it different is that abnormal blood vessels grow under the retina where they do not belong. These vessels are fragile. They leak blood and fluid right into the macula, and the damage happens fast. Wet AMD can cause irreversible vision loss in a short amount of time if nobody catches it. Treatment usually means injections of anti-VEGF drugs into the eye to stop the leaking. Wet AMD requires constant monitoring because it can flare up without warning.
Something people do not always realize: you can start out with dry age-related macular degeneration and it can turn into the wet form later. That shift can happen at any stage. Nobody can predict exactly when or if it will happen, which is part of why macular degeneration keeps people on edge.
Risk factors? Age is number one. After that, smoking, family history, genes, high blood pressure, and too much UV exposure over the years. If macular degeneration runs in your family you should be paying extra attention as you get older.
Your eye doctor might also hand you something called an amsler grid. Just a piece of paper with a bunch of straight lines and a dot in the middle. You stare at the dot and see if any lines look wavy or bent or missing. If they do, something might be shifting with your macular degeneration and you need to call your doctor. Simple tool. But it catches things between appointments that you might otherwise miss.
Why Vision Loss Goes Beyond What Injections Can Fix
If you have wet AMD your doctor probably has you on injections already. And they work. They slow the leaking and protect your vision from dropping off a cliff. Nobody is knocking that.
But here is what the injections do not do. They do not fix the macula itself. They do not bring back cells that already died. They do not touch the deeper damage underneath. And if you have dry age-related macular degeneration? There is no injection for that at all. You get supplements, maybe some lifestyle advice, and a lot of monitoring. But no medical treatment that actually reverses the atrophy that is eating away at your macula.
So what keeps macular degeneration getting worse even when you are doing everything your doctor told you?
Three things, mainly. Chronic inflammation inside the eye. It breaks down the membrane under the macula and speeds up cell death. Oxidative stress, which is basically your body creating waste faster than it can take the garbage out. That gets worse as you age. And bad circulation, meaning the macula is not getting enough blood, not enough oxygen, not enough of what it needs to hang on.
Those three problems drive macular degeneration forward regardless of whether you have the dry type or the wet type. Injections were never designed to deal with them. Nutritional support covers part of it but not the whole picture. That is where acupuncture comes in.
How Ophthalmic Acupuncture Works for AMD
People always ask about the needles so let me just say it. No needles go in the eyes. Not near them either. The points we use for macular degeneration treatment sit around the brow bone, the temples, and the orbital rim, which is that bony ridge circling your eye socket. Then there are points on the hands, arms, and legs that deal with circulation, inflammation, and the organ systems that Traditional Chinese Medicine ties to vision and overall eye health.
We are not trying to replace your ophthalmologist. Your injections stay. Your other treatments stay. What acupuncture does is tackle the parts of macular degeneration that everything else misses. The inflammation that will not quit. The poor blood flow to the retina. The oxidative stress that keeps piling up. Those are the things pushing macular degeneration forward and they are the things nobody else on your care team is directly going after.
What do our macular degeneration patients actually notice? In our clinic people tell us their vision feels more stable. Some say their central vision got a bit sharper over a few months. Others say the blurry spots or dark patches just stopped spreading. We track every case and line our findings up with whatever your eye doctor is reporting at your regular visits.
I am not going to sit here and call this a miracle. Macular degeneration is serious and it does not go away. But layering acupuncture on top of your existing macular degeneration care gives you one more way to fight back. And it goes after root causes instead of just managing what is already gone wrong.
How Ophthalmic Acupuncture Treats Macular Degeneration
A 2023 review in Medicine pulled together data from multiple clinical trials on acupuncture for age-related macular degeneration. Patients who added acupuncture to their existing macular degeneration treatment saw real improvements in visual acuity and retinal health. The best outcomes showed up in people who combined acupuncture with their conventional macular degeneration care, not the ones doing acupuncture by itself.
Other research has backed this up. Acupuncture appears to improve circulation to the retina and dial down the chronic inflammation that keeps macular degeneration progressing.
The bigger picture is this. Age-related macular degeneration hits millions of people worldwide. It does not fix itself. But the people who catch macular degeneration early and attack it from more than one angle tend to keep more of their vision for longer. Your risk factor management, your eye exams, your medical care, plus something that actually addresses the inflammation and circulation issues underneath. That combination works better than any single approach on its own.
If macular degeneration is part of your life right now, whether dry or wet, early or advanced ARMD, and you are ready to do more than just sit and watch it progress, get in touch with Honor Wellness. Book a consultation. Your vision is not something you get back once it is gone, so the earlier you start treating macular degeneration from every angle the better off you are going to be.
Frequently Asked Questions
How long does it typically take for macular degeneration to progress to significant vision loss?
How long it takes for macular degeneration to progress to significant vision loss varies greatly depending on the type and stage of the condition at the time of diagnosis. Dry macular degeneration, which is the most common form, tends to progress slowly over many years and decades, with some patients experiencing only gradual and minimal central vision changes throughout their lifetime. Wet macular degeneration however can progress much more rapidly, sometimes causing significant central vision loss within weeks or months without prompt treatment. Early detection, consistent monitoring, targeted nutrition, and regular acupuncture treatments that improve retinal blood flow are all essential in slowing progression and preserving vision for as long as possible.
What dietary choices should be avoided by someone with macular degeneration?
Several dietary choices should be avoided by someone with macular degeneration as they promote inflammation and oxidative stress that accelerate retinal degeneration. Processed foods, refined sugars, trans fats, and foods high in saturated fat have all been associated with worsening macular health. Excessive alcohol consumption and a diet low in fresh vegetables, antioxidants, and omega 3 fatty acids also contribute negatively to retinal health over time. Focusing on a nutrient rich anti inflammatory diet abundant in leafy greens, colorful vegetables, oily fish, and foods rich in lutein and zeaxanthin provides the retina with the nutritional support it needs to function and maintain itself as effectively as possible.Is it still safe to drive with macular degeneration affecting only one eye?
Is it still safe to drive with macular degeneration affecting only one eye?
Whether it is safe to drive with macular degeneration affecting only one eye depends on the degree of central vision loss in the affected eye and the quality of vision in the unaffected eye. In many early cases where the unaffected eye compensates effectively, some patients are still able to drive safely and legally. However as the condition progresses or begins to affect the second eye, driving safety becomes increasingly compromised. Regular vision assessments with a qualified eye care professional are essential and legally required in most regions to determine whether driving remains safe and appropriate for your specific level of visual function.
What activities and habits should be avoided when managing macular degeneration?
When managing macular degeneration there are several important activities and habits to avoid in order to protect the macula and slow the progression of retinal damage. Smoking is one of the most significant risk factors and should be eliminated entirely as it dramatically accelerates macular degeneration by reducing blood flow and increasing oxidative damage to the retina. Prolonged exposure to UV light and high energy blue light without protective eyewear, a diet high in processed and inflammatory foods, unmanaged cardiovascular risk factors, and chronic stress should all be actively avoided. Maintaining a healthy lifestyle, attending regular monitoring appointments, and supporting retinal health through acupuncture and targeted nutritional supplementation are all essential components of responsible long term macular degeneration management.
What other eye conditions can produce symptoms similar to macular degeneration?
Several other eye conditions can produce symptoms similar to macular degeneration and should be carefully distinguished through a comprehensive eye examination. Central serous chorioretinopathy, diabetic macular edema, epiretinal membrane, Stargardt disease, and macular holes can all cause central vision distortion, blurring, and difficulty with detailed tasks that closely resemble the symptoms of macular degeneration. Certain medications including hydroxychloroquine used for autoimmune conditions can also cause macular toxicity that mimics the appearance of macular degeneration on examination. An accurate diagnosis from a qualified eye care professional using imaging technology such as optical coherence tomography is essential to ensure the correct condition is identified and the most appropriate and effective treatment plan is put in place.
